Heart blockage is one of the most common and serious heart conditions affecting people today. It happens when the arteries that supply blood to your heart become narrowed or blocked due to plaque build-up — a condition known as coronary artery disease. When blood flow to the heart is reduced, your heart cannot work properly, and over time, this can lead to chest pain, breathlessness, or even a heart attack.
The good news is that heart blockage treatment has advanced significantly over the years. Whether your condition is mild or severe, there are proven medical options available — from medications and lifestyle changes to angioplasty, stenting, and bypass surgery. With the right care at the right time, most patients are able to recover well and live an active, healthy life.
Dr. Karthick Sabapathi is an experienced interventional cardiologist based in Chennai who specialises in the diagnosis and treatment for blocked arteries. With over 15 years of focused cardiac practice and thousands of successful procedures, Dr. Karthick Sabapathi offers patients a personalised, evidence-based approach to coronary heart disease — from the very first consultation through to long-term recovery and prevention.
Understanding Heart Blockage Treatment
What Is Heart Blockage?
Your heart works every second of your life, and it needs a steady supply of blood to keep going. That blood is delivered through the coronary arteries — a network of vessels that wraps around your heart. When those arteries get blocked or narrowed, your heart muscle does not receive enough blood and oxygen. This is what doctors call a heart blockage.
Over time, a waxy substance called plaque — made up of cholesterol, fat, and calcium — builds up on the inner walls of these arteries. As plaque accumulates, the artery becomes narrower and blood flow slows down. If a piece of plaque breaks open, a blood clot can form and block the artery completely, triggering a heart attack. Effective heart blockage treatment aims to restore that blood flow and protect your heart.
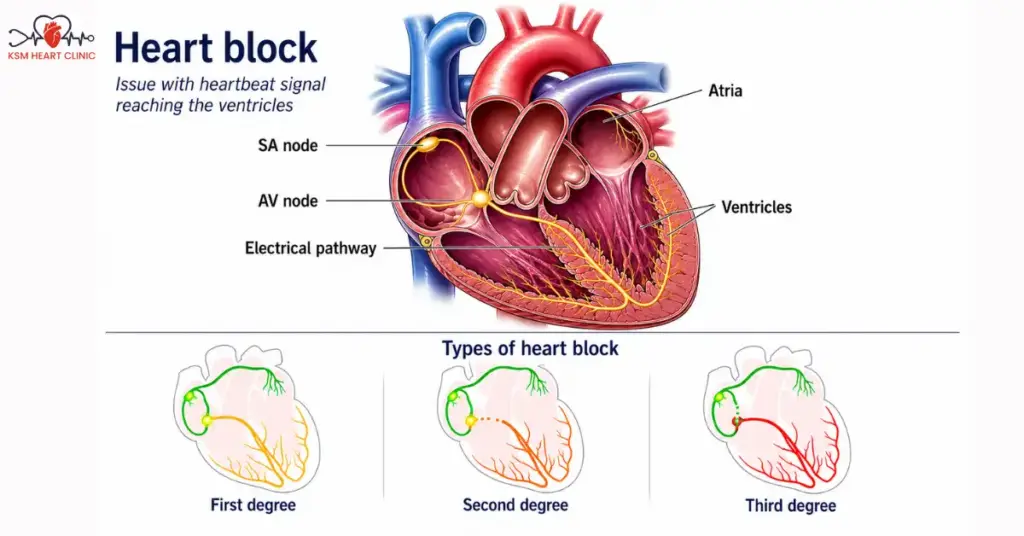
Causes and Risk Factors of Heart Blockage
Heart blockage does not happen overnight. It is usually the result of years of unhealthy habits and underlying health conditions working together. Some of the most common contributing factors include:
- High cholesterol — excess LDL cholesterol sticks to artery walls and gradually forms plaque.
- High blood pressure — puts extra force on artery walls, making them more prone to damage.
- Type 2 diabetes — raised blood sugar levels can damage blood vessels over time.
- Smoking — chemicals in tobacco cause inflammation in the arteries and speed up plaque build-up.
- Obesity — excess body fat is linked to higher cholesterol, blood pressure, and blood sugar levels.
- Sedentary lifestyle — physical inactivity weakens the heart and raises risk factors for blockage.
- Family history — if a close relative has had coronary heart disease, your own risk is higher.
Age and gender — men above 45 and women above 55 face a gradually increasing risk.
Understanding what puts you at risk is the first step toward preventing and managing coronary artery disease.
Symptoms That Indicate a Heart Blockage
One of the challenges with heart blockage is that it can be silent for many years. In some people, the first sign is a heart attack. However, for many patients, there are warning signals the body sends out that should never be ignored.
- Chest pain or tightness, especially during physical activity
- Shortness of breath even with mild effort
- Unexplained fatigue or sudden tiredness
- Irregular heartbeat or palpitations
- Nausea, dizziness, or cold sweats
- Pain radiating to the arm, jaw, or neck
These symptoms — especially chest discomfort during exercise — are signs that your heart is under stress. The moment you notice them, it is time to speak with a cardiologist. The earlier a blockage is found, the more treatment options are available and the better the outcome.
Importance of Early Diagnosis and Treatment
Catching a heart blockage early makes a significant difference. When the blockage is small and the artery is only partially narrowed, doctors can often manage it with medication and lifestyle changes alone. As blockages worsen, more involved procedures like angioplasty or bypass surgery may become necessary.
Early diagnosis also gives you time to make real changes — to your diet, your activity level, and your health habits — that can slow or even stop the progression of the disease. Dr. Karthick Sabapathi emphasizes that most patients who come in at the right time benefit enormously from a well-planned heart blockage treatment strategy built around their specific condition.
Types of Heart Blockage Conditions
Partial vs Complete Artery Blockage
Not all blockages are the same. A partial blockage means the artery is narrowed but blood can still flow through — though in reduced amounts. This is called a stenosis, and it can cause symptoms during physical exertion when the heart demands more blood than the narrowed artery can supply.
A complete blockage means blood flow through that artery has stopped entirely. This is a medical emergency and often results in a heart attack. The tissue supplied by that artery starts dying within minutes if flow is not restored. This is precisely why timely heart blockage treatment — whether through clot-busting medication or emergency angioplasty — is so critical.
Coronary Artery Disease and Heart Blockage
Coronary artery disease (CAD) is the most common form of heart disease worldwide, and heart blockage is its defining feature. In CAD, the coronary arteries that supply blood to the heart muscle slowly become hardened and narrowed due to plaque build-up — a process called atherosclerosis.
Over years, this process can go undetected. Many patients first learn they have coronary artery disease only after experiencing angina (chest pain) or a heart attack. Managing CAD requires a long-term strategy that includes both medical treatment and meaningful lifestyle changes.
Single, Double, and Triple Vessel Disease
The term “vessel disease” refers to how many coronary arteries are affected by significant blockages.
- Single vessel disease — one artery is significantly blocked. Often treated with angioplasty and stenting.
- Double vessel disease — two arteries are involved. Treatment depends on the severity and location of blockages.
- Triple vessel disease — all three major coronary arteries are affected. This is more serious and often requires bypass surgery.
The choice of treatment is tailored to each patient. Dr. Karthick Sabapathi carefully evaluates which arteries are blocked, to what extent, and which approach will best protect heart function over time.
Chronic vs Sudden Heart Blockage
A chronic blockage develops slowly over years. The heart often adapts by growing small collateral vessels that partially compensate for reduced blood flow. Symptoms may be mild and manageable for a long time.
A sudden blockage happens rapidly — usually when a plaque ruptures and a blood clot forms instantly. This triggers an acute heart attack and requires immediate medical intervention. Time is muscle: every minute of delay allows more heart tissue to be damaged permanently.
Diagnosis of Heart Blockage
Physical Examination and Medical History
The diagnostic process begins with a conversation. Dr. Karthick Sabapathi will ask about your symptoms, how long you have had them, what makes them better or worse, and your complete medical history. He will also ask about your family history of heart disease, lifestyle habits, and any medications you take.
A physical examination will check your blood pressure, heart rate, and listen to your heart and lungs. This first step helps the doctor understand your overall risk profile and guides which tests to order next.
Blood Tests and Cholesterol Screening
Blood tests provide important information about your heart health. A lipid panel measures total cholesterol, LDL, HDL, and triglyceride levels. High LDL cholesterol is one of the strongest predictors of coronary artery disease. Blood glucose and HbA1c tests check for diabetes. During a suspected heart attack, troponin levels in the blood rise quickly and confirm whether heart muscle damage has occurred.
ECG and Stress Testing
An electrocardiogram (ECG) records the electrical signals in your heart and is one of the quickest ways to detect abnormal heart rhythms or signs of reduced blood flow. It is painless and takes only a few minutes.
A stress test (also called a treadmill test) goes one step further. You walk on a treadmill while your heart’s electrical activity and blood pressure are monitored. As your heart works harder, any blockage-related problems in blood supply become more apparent.
Echocardiogram and Cardiac Imaging
An echocardiogram uses sound waves to create a moving picture of your heart. It shows how the heart chambers and valves are working, how strongly the heart is pumping (ejection fraction), and whether certain walls of the heart are moving abnormally — which can point to areas with reduced blood flow.
More advanced imaging such as a CT coronary angiogram can show the coronary arteries in detail and reveal calcification or narrowing without the need for a procedure.
Angiography for Detecting Blockages
Coronary angiography is considered the gold standard for diagnosing blocked arteries. A thin, flexible tube called a catheter is guided to the coronary arteries. A special contrast dye is injected, and X-ray images clearly show exactly where the blockages are, how severe they are, and how many arteries are involved.
This procedure typically takes 30 to 60 minutes and is done under local anesthesia. Patients are awake but relaxed. If a significant blockage is found, the doctor may proceed with angioplasty and stenting in the same session, addressing the problem immediately.
Heart Blockage Treatment Options
The right heart blockage treatment depends on the number of arteries affected, the severity of blockages, the patient’s overall health, and other individual factors. There is no single approach that works for everyone. Here is an overview of what is available.
Lifestyle Changes and Risk Management
For patients with mild to moderate coronary artery disease, targeted lifestyle changes can be remarkably effective. Switching to a heart-healthy diet, exercising regularly, achieving and maintaining a healthy weight, and quitting smoking all work together to reduce the rate at which plaque builds up in the arteries.
These changes are also essential even after more advanced treatments like angioplasty or bypass surgery. Without addressing the underlying risk factors, blockages can recur. Lifestyle management is not a one-time effort — it is an ongoing commitment to heart health.
Medications for Heart Blockage Treatment
Medications are a cornerstone of the diagnosis and treatment for blocked arteries. They work in different ways to protect your heart:
- Statins — reduce LDL cholesterol and stabilize plaque, making it less likely to rupture.
- Antiplatelet drugs (like aspirin or clopidogrel) — prevent blood clots from forming on plaque.
- Beta-blockers — slow the heart rate and reduce the heart’s workload, easing chest pain.
- ACE inhibitors / ARBs — lower blood pressure and protect the heart muscle from further damage.
- Nitrates — relax and widen the blood vessels, relieving chest pain quickly.
- Calcium channel blockers — help relax artery walls and reduce the heart’s oxygen demand.
Angioplasty and Stent Placement
Percutaneous coronary intervention (PCI) — commonly known as angioplasty — is one of the most commonly performed procedures for heart blockage treatment. During the procedure, a tiny balloon is threaded to the blocked artery and inflated to compress the plaque and widen the artery. A stent — a small mesh tube — is then placed inside the artery to keep it open.
Modern drug-eluting stents slowly release medication that prevents the artery from narrowing again. The procedure is minimally invasive, done through a small puncture at the wrist or groin, requires no general anesthesia, and patients typically go home within one to two days.
Bypass Surgery (CABG)
Coronary artery bypass grafting (CABG) is a surgical procedure that creates a new path for blood to flow around a blocked section of the artery. The surgeon takes a healthy blood vessel — usually from the chest wall, leg, or arm — and attaches it above and below the blocked area, effectively bypassing the blockage.
CABG is generally recommended for patients with multiple severe blockages, triple vessel disease, or blockages in the left main coronary artery. Results are excellent and can provide relief from symptoms for many years.
Minimally Invasive Heart Procedures
Advances in cardiac care have made it possible to treat certain heart conditions through smaller incisions and with less recovery time. Minimally invasive bypass surgery, robotic-assisted procedures, and hybrid approaches give surgeons and cardiologists more options to tailor treatment to each patient’s anatomy and medical condition.
Non-Surgical Treatments for Heart Blockage
Diet and Nutrition Changes
What you eat has a direct impact on your heart and arteries. A heart-healthy diet is one of the most powerful non-surgical tools available. Focus on:
- Plenty of vegetables, fruits, and whole grains — rich in fiber, which helps lower cholesterol.
- Lean proteins like fish, legumes, and low-fat dairy rather than red and processed meats.
- Healthy fats from olive oil, nuts, and avocado — replacing saturated and trans fats.
- Reduced sodium to help control blood pressure.
- Limited added sugars and refined carbohydrates, which contribute to weight gain.
The Mediterranean diet in particular has a strong evidence base for reducing the risk and progression of coronary heart disease. Small, consistent changes to daily eating habits add up to significant benefits.
Exercise and Cardiac Rehabilitation
Physical activity is medicine for the heart. Regular moderate exercise — such as brisk walking, cycling, or swimming for 30 minutes on most days of the week — strengthens the heart muscle, lowers blood pressure, improves cholesterol levels, helps manage weight, and reduces stress.
Cardiac rehabilitation is a structured program designed for people recovering from a heart event or procedure. It combines supervised exercise sessions, education about heart-healthy living, and psychological support. Patients who complete cardiac rehabilitation show better recovery and fewer repeat heart events.
Controlling Blood Pressure and Diabetes
High blood pressure and diabetes are two of the most damaging conditions for coronary arteries. Both significantly accelerate the development of coronary artery disease. Bringing blood pressure below 130/80 mmHg — through medication, diet, and exercise — meaningfully reduces the strain on arterial walls. Managing blood sugar through medication, a low-glycaemic diet, and regular monitoring protects the inner lining of blood vessels from chronic damage.
Smoking Cessation and Stress Management
Smoking is one of the single most damaging habits for heart health. It raises blood pressure, reduces good cholesterol, increases clotting tendency, and directly damages the lining of the arteries. Quitting smoking — even later in life — rapidly reduces the risk of future heart events.
Chronic stress triggers the release of hormones like cortisol and adrenaline that raise blood pressure and inflammation. Techniques such as mindfulness, yoga, deep breathing, adequate sleep, and social connection all support a lower-stress, heart-healthy lifestyle.
Surgical Treatments for Severe Heart Blockage
When Surgery Is Recommended
Surgery is considered when blockages are too severe, too numerous, or too complex to be safely treated with angioplasty and stenting alone. Specific situations where bypass surgery is typically recommended:
- Blockage in the left main coronary artery (which supplies 40% or more of blood to the heart)
- Triple vessel disease with reduced heart function
- Blockages that are too long or calcified for effective stenting
- Angioplasty results that failed and the artery re-narrowed
- Patients with diabetes and multi-vessel disease, where surgery offers better long-term outcomes
The decision to operate is never made lightly. It involves a careful review of angiography findings, heart function tests, patient health, and a detailed discussion between the patient and their cardiac team.
Coronary Artery Bypass Surgery Procedure
In a standard CABG operation, the patient is placed under general anesthesia. The surgeon opens the chest and temporarily connects the patient to a heart-lung bypass machine that keeps blood circulating during the procedure. Healthy blood vessel grafts — taken from the chest wall artery, leg vein, or arm artery — are sewn above and below each blocked segment, creating new pathways for blood to reach the heart muscle.
The surgery typically takes 3 to 5 hours. The number of bypasses performed corresponds to the number of severely blocked arteries — single, double, triple, or even quadruple bypass.
Recovery After Heart Surgery
After bypass surgery, patients spend 1 to 2 days in the intensive care unit for monitoring, followed by an additional 5 to 7 days in a general cardiac ward. Most patients return home within a week. Full recovery typically takes 6 to 12 weeks depending on overall health, age, and complexity of the surgery.
During recovery, it is important to follow wound care instructions carefully, take all prescribed medications, participate in cardiac rehabilitation, and attend all follow-up appointments. Most patients experience significant improvement in symptoms within a few weeks.
“Surgery is not the end of the journey — it is the beginning of a healthier chapter. Patients who commit to their aftercare consistently achieve excellent long-term outcomes.”
Risks and Benefits of Surgical Treatment
Like all surgical procedures, CABG carries certain risks — including infection, bleeding, stroke, kidney problems, or irregular heart rhythms in the immediate post-operative period. However, in the right patients, the benefits of surgery far outweigh these risks. CABG reliably relieves symptoms, significantly improves blood flow to the heart, reduces the risk of heart attack, and can extend life expectancy for patients with severe multi-vessel disease.
Recovery and Aftercare Following Treatment
Post-Treatment Lifestyle Adjustments
Recovery from heart blockage treatment is as much about changing daily habits as it is about physical healing. After angioplasty or bypass surgery, your heart needs time to recover — but it also needs the right environment to stay healthy long-term. This means adopting a heart-healthy diet, becoming physically active in a gradual and supervised way, and taking all prescribed medications consistently.
Driving is usually restricted for two to four weeks after bypass surgery and for a shorter period after angioplasty. Returning to work depends on the type of job — most people with desk jobs resume within four to eight weeks after surgery.
Follow-Up Care and Monitoring
Regular follow-up appointments with Dr. Karthick Sabapathi are essential after any heart procedure. These visits typically involve reviewing symptoms, performing an ECG, checking blood pressure, repeating blood tests to assess cholesterol and glucose levels, and evaluating how well medications are working.
An echocardiogram may be repeated periodically to track heart function. In some patients, a repeat stress test or imaging study is done at specific intervals to check whether treated arteries remain open.
Medications After Treatment
After angioplasty and stenting, patients are placed on dual antiplatelet therapy — typically aspirin along with clopidogrel or a similar drug — for a set period (often 6 to 12 months) to prevent clots forming around the stent. After bypass surgery, aspirin is generally continued long-term. Statins, blood pressure medications, and other heart drugs are also continued as they protect against future events.
Never stop taking heart medications without consulting your doctor, even if you feel completely well. These medications are doing important protective work even when you cannot feel them working.
Preventing Future Heart Blockages
A treated heart blockage is not a cured heart condition. The underlying process — atherosclerosis — continues unless you actively work to control your risk factors. With proper management, the progression of coronary heart disease can be significantly slowed or halted.
Prevention Checklist — Key Steps After Treatment
- Take all medications exactly as prescribed — never skip doses
- Eat more vegetables, fruits, whole grains, and lean protein
- Walk briskly for at least 30 minutes on most days of the week
- Check and control your blood pressure and blood sugar regularly
- Quit smoking — ask your doctor for support if needed
- Manage stress through relaxation, good sleep, and social support
- Attend every follow-up appointment without fail
Choosing the Right Heart Specialist
Role of a Cardiologist in Treatment
A cardiologist is a specialist physician trained specifically in diagnosing and treating diseases of the heart and blood vessels. For patients with coronary heart disease or blocked arteries, a cardiologist coordinates all care — from ordering the right diagnostic tests to recommending treatment and managing long-term follow-up.
An interventional cardiologist like Dr. Karthick Sabapathi has advanced training in catheter-based procedures such as angioplasty and stenting. The same specialist who interprets your angiogram can also perform the procedure to fix the problem, ensuring continuity of care.
Importance of Specialized Cardiac Care
Cardiac care is not a one-size-fits-all field. Decisions about whether to stent, bypass, or manage a blockage medically require expertise, experience, and access to advanced diagnostic equipment. A specialist who performs a high volume of cardiac procedures consistently achieves better outcomes — not just because of technical skill, but because of deep clinical judgment built over years of practice.
Questions to Ask Before Treatment
Being informed and involved in your own treatment decisions leads to better outcomes. Before starting any treatment for coronary artery disease, consider asking your cardiologist:
- How many arteries are blocked, and how severe are the blockages?
- What are my treatment options — and which do you recommend for me specifically?
- What are the risks and benefits of each option?
- Will medication and lifestyle changes alone be sufficient, or is a procedure necessary?
- How long will recovery take, and when can I return to normal activities?
- How often will I need follow-up appointments?
A good cardiologist welcomes these questions and takes time to explain the reasoning behind every recommendation clearly.
Conclusion
When it comes to heart health, the quality of the care team and facilities matters enormously. Look for a cardiologist with proven experience in interventional procedures, access to modern catheterization laboratories, and a strong track record of patient outcomes. Dr. Karthick Sabapathi brings years of specialized experience in the diagnosis and treatment for blocked arteries, offering patients in Chennai access to comprehensive, world-class cardiac care with a deeply personal approach.