Every year, thousands of lives are lost simply because people didn’t recognize the symptoms of heart attack in time. And honestly? That’s heartbreaking because most of these signs are things we can learn. The tricky part is that the symptoms of heart attack aren’t always dramatic. Sometimes they show up as something as ordinary as feeling tired, a little nauseous, or slightly short of breath. Symptoms of Heart Attack That’s exactly why we’re talking about this today. The more you know about the symptoms of heart attack, the better equipped you are to act fast when it matters most.
What Is a Heart Attack?
Understanding Myocardial Infarction in Simple Terms
A heart attack — medically called a myocardial infarction (MI) — happens when the blood supply to part of the heart muscle gets cut off. When heart muscle cells don’t receive the oxygen-rich blood they need, they start to die within minutes. Time is absolutely critical here. The faster the blood flow is restored, the more of the heart muscle can be saved.
The heart is a powerful pump that works 24 hours a day. It gets its own blood supply through a network of arteries called the coronary arteries. When one of these arteries gets blocked — usually by a blood clot sitting on top of a fatty buildup inside the artery wall — a heart attack begins. This is why recognizing the symptoms of heart attack early can genuinely save your life or the life of someone around you.
How Blood Flow Blockage Affects the Heart
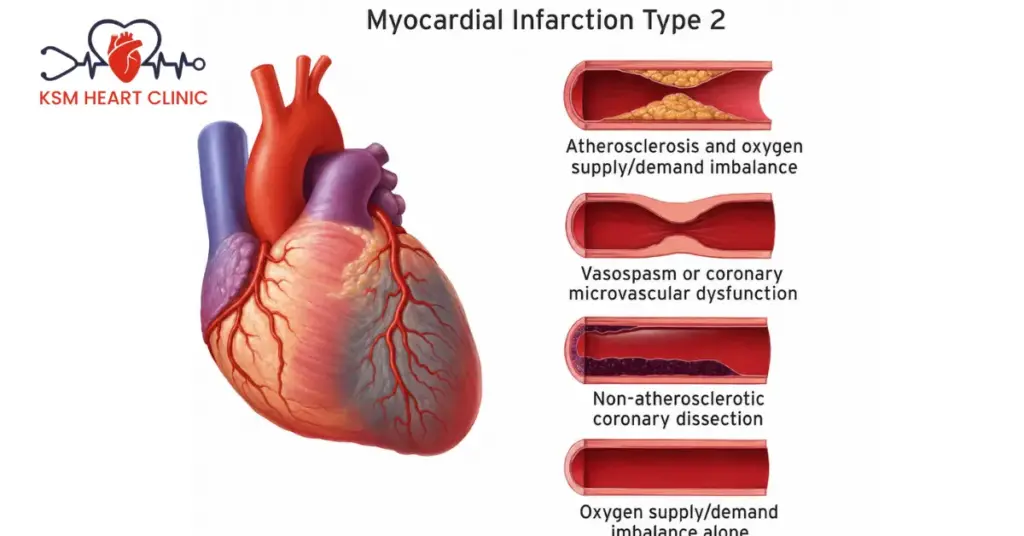
Fatty deposits called plaques form inside the coronary artery walls over years, slowly narrowing the passage. When a plaque becomes unstable and ruptures, the body responds by forming a blood clot around it. This clot can grow large enough to completely block blood flow through the artery. The part of the heart muscle that depends on that artery then loses its oxygen supply and begins to suffer damage — that damage is what we call a heart attack.
The longer the blockage stays in place, the more muscle tissue is lost. This is why doctors and emergency teams often say: time is muscle. Every minute matters from the moment the first symptom appears.
Common Symptoms of Heart Attack
The common symptoms of heart attack can range from dramatic and unmistakable to surprisingly mild. Some people experience intense, crushing chest pain. Others feel a dull discomfort they might easily ignore. Knowing the full range helps you respond appropriately — whether it’s you, a family member, or a colleague.
Chest Pain or Discomfort
Chest pain is the most widely recognized of all the symptoms of heart attack. People often describe it as a heavy weight pressing down on the chest, a tight squeezing sensation, or a burning feeling. The discomfort is usually felt in the centre or left side of the chest and may last more than a few minutes. It can come and go, or it may stay constant. If the chest discomfort is accompanied by any other symptom on this list, do not wait — seek help immediately.
It’s worth noting that the chest discomfort doesn’t always feel like sharp pain. Some people describe it as a fullness or tightness rather than pain. Never dismiss this feeling as something minor if it lingers or is accompanied by other warning signs.
Pain in Arm, Neck, Jaw, or Back
The heart is connected to a network of nerves, and when it is in distress, the pain can radiate to other parts of the body. Most commonly, pain travels down the left arm — though it can also affect the right arm. Some people feel a strange aching in the jaw, the back of the neck, or between the shoulder blades. This referred pain happens because the brain sometimes misinterprets where the distress signal is coming from.
If you feel an unusual ache in your jaw, inner arm, or upper back that you cannot explain — especially if it comes with chest discomfort or breathlessness — treat it seriously.
Shortness of Breath
When the heart is struggling to pump blood effectively, the lungs can get congested. This makes breathing feel laboured or difficult, even when the person is sitting still. Shortness of breath can occur before chest pain appears, or it may be the only major symptom in some individuals — particularly women. If you find yourself suddenly unable to take a full, comfortable breath for no clear reason, it deserves prompt attention.
Cold Sweating
A sudden cold sweat — one that breaks out without physical activity or heat — is a classic warning sign. The body’s emergency stress response releases hormones that trigger this reaction when the heart is under severe stress. Unlike the normal sweating from exercise or warmth, this sweat feels clammy and comes out of nowhere. Combined with other symptoms, it is a strong signal that something serious may be happening.
Nausea or Vomiting
Feeling nauseated or actually vomiting during or before a heart attack is more common than most people realize, particularly in women. The connection between the heart and the digestive system through the vagus nerve means cardiac distress can trigger gut symptoms. Many people who have suffered heart attacks report thinking they had food poisoning or severe indigestion at the time. If nausea arrives alongside chest pressure or cold sweat, do not brush it off as a stomach issue.
Dizziness or Lightheadedness
A sudden drop in blood pressure or an irregular heartbeat during a cardiac event can reduce blood flow to the brain. This leads to dizziness, a spinning sensation, or the feeling that you are about to faint. Sometimes people briefly lose balance or feel their head go suddenly light. While dizziness alone has many possible causes, when it appears together with chest discomfort or cold sweat, it strongly points to a cardiac emergency.
Early Warning Signs of a Heart Attack
One of the most valuable things you can learn is that the body often gives warning signals days or even weeks before a full heart attack occurs. These early symptoms of heart attack are easy to overlook because they feel so ordinary. Paying attention to them can give you time to seek medical advice before an emergency happens.
Mild Chest Discomfort
In the days leading up to a heart attack, some people notice a mild, occasional discomfort in the chest. It might come and go quickly and feel more like a brief twinge or slight pressure rather than serious pain. Because it passes so fast, many people ignore it or attribute it to stress or muscle tension. If this discomfort is new, keeps returning, or comes on with mild activity, discuss it with a cardiologist without delay.
Unusual Fatigue
Feeling unusually tired without a clear reason is one of the most frequently missed pre-warning symptoms of a heart attack, especially among women. When the heart has to work harder to pump blood through a partially blocked artery, the body consumes more energy just to keep going. A person may feel exhausted after small tasks — like climbing a short flight of stairs — that never used to cause any problem. This kind of unexplained tiredness lasting several days is a reason to see a doctor.
Indigestion-Like Feeling
A burning sensation in the upper abdomen or chest, similar to heartburn or acid reflux, can be an early cardiac symptom. The problem is that it genuinely feels like a digestive issue. Many people reach for antacids and wait for it to pass, not realizing it could be their heart sending distress signals. If this burning or indigestion-like discomfort appears together with fatigue, mild breathlessness, or cold sweat — even mildly — it should not be dismissed.
Sleep Disturbances
Difficulty sleeping, waking up repeatedly through the night, or feeling unusually anxious at bedtime has been reported by heart attack survivors as something that occurred in the weeks before the event. The exact reason is not fully understood, but it may be related to the body’s stress response activating at night as the cardiovascular system struggles. If you are sleeping badly without a clear reason, and especially if any of the other early symptoms are also present, it is worth getting your heart checked.
Symptoms of Heart Attack in Men vs Women
Heart disease is not just a man’s concern. It affects women just as significantly — but often in less obvious ways. Understanding the differences in how the symptoms of heart attack present in men and women can be life-saving, particularly because women’s symptoms are often attributed to other causes and treatment can be delayed.
Common Symptoms in Men
Men more frequently experience the “classic” presentation: a sudden, intense chest pain or tightness that may radiate to the left arm or jaw. They often break into a cold sweat, feel severe shortness of breath, and may feel dizzy or faint. Because these symptoms match what most people picture as a heart attack, men tend to recognize them more readily and seek help faster. However, even men can have atypical presentations, so no symptom should be dismissed simply because it doesn’t fit the classic pattern.
Subtle Symptoms in Women
Women are more likely to experience symptoms that don’t immediately scream “heart attack.” These include extreme fatigue that can last for days, pressure or discomfort in the upper back, neck, or jaw (rather than the chest), nausea, vomiting, and shortness of breath without significant chest pain. Some women describe a sense of crushing fatigue or feeling deeply unwell before a cardiac event, rather than the dramatic chest-clutching moment depicted in films.
These early symptoms of heart attack in women are often mistaken for anxiety, stress, or digestive problems — which means treatment is sometimes delayed. Women who notice any combination of these unusual symptoms should take them seriously and seek prompt evaluation.
Why Symptoms Differ Between Genders
The biological differences between male and female hearts partly explain the symptom differences. Women tend to develop blockages in the smaller coronary arteries (a condition called microvascular disease) rather than only in the large main arteries. This can produce a different pattern of pain and discomfort. Hormonal factors, particularly the protective role of oestrogen before menopause, also affect how heart disease develops and presents. After menopause, women’s cardiac risk increases significantly, and their symptoms can become more pronounced.
Silent Heart Attack Symptoms
What Is a Silent Heart Attack?
A silent heart attack — medically known as a silent myocardial infarction (SMI) — is a heart attack that occurs without the person being aware of it at the time. There is no dramatic chest-clutching moment. The person may feel vaguely unwell for a short time, or nothing at all. The damage to the heart muscle still happens, just like in a typical heart attack, but because the symptoms are so mild or unusual, they go unrecognized.
Silent heart attacks are often discovered only later — during a routine ECG or cardiac checkup — when changes to the heart’s electrical activity reveal that a previous event occurred. This is why regular cardiac screening is so important, even if you feel generally well.
Symptoms That Often Go Unnoticed
The symptoms of a silent heart attack may include mild discomfort in the chest or upper body that is easy to attribute to muscle strain or indigestion, brief bouts of breathlessness or fatigue, a fleeting feeling of nausea, and general discomfort that passes quickly. Because each of these feels like something ordinary, most people do not connect them to their heart. The subtlety is precisely what makes silent heart attacks dangerous — the heart has been damaged, but no one has intervened.
High-Risk Groups (Diabetes, Elderly)
People with diabetes are at particularly high risk for silent heart attacks. High blood sugar over time can damage the nerves that would normally carry pain signals from the heart to the brain — this is called cardiac autonomic neuropathy. As a result, a diabetic individual may have a significant cardiac event without feeling the chest pain that would alert most people. The elderly are also more vulnerable because they may attribute symptoms like fatigue or breathlessness to aging rather than to a cardiac cause.
Important for Diabetics and the Elderly
If you or a loved one has diabetes or is above 60, schedule regular cardiac checkups even in the absence of symptoms. Silent damage to the heart can be detected early and treated effectively.
When to Seek Emergency Medical Help
Call Emergency Services Immediately If You Experience:
Chest pain or pressure lasting more than 2 minutes, shortness of breath with chest discomfort, sudden cold sweating alongside any other symptom, pain spreading to the arm, jaw, or back, or sudden dizziness or near-fainting.
Warning Signs That Need Immediate Attention
If chest discomfort — whether mild or intense — lasts more than two minutes or comes and goes repeatedly, this is a medical emergency. Don’t wait to see if it passes on its own. Don’t drive yourself to the hospital if you can avoid it. Call emergency services immediately. The faster a blocked artery is opened (usually through a procedure called primary angioplasty), the more heart muscle is preserved and the better the recovery.
Other urgent signs include sudden extreme weakness, confusion, or the inability to stay upright. These can indicate that the heart is severely compromised and blood flow to the brain is being affected. Any combination of two or more of the symptoms described in this article — particularly if they came on suddenly — should be treated as a cardiac emergency.
Difference Between Heart Attack and Cardiac Arrest
These two terms are often confused, but they describe different events. A heart attack is a circulation problem — a blocked artery cuts off blood supply to the heart muscle. The person is usually conscious, in pain or discomfort, and the heart is still beating (though struggling). A cardiac arrest, on the other hand, is an electrical problem — the heart suddenly stops beating altogether. The person collapses immediately, becomes unresponsive, and stops breathing normally.
A heart attack can trigger a cardiac arrest, which is why rapid treatment is so critical. However, cardiac arrest can also occur independently. In the case of cardiac arrest, CPR and a defibrillator are needed immediately. In the case of a heart attack, emergency medical treatment to restore blood flow is the priority.
What to Do During a Heart Attack
Immediate First Aid Steps
Step 1 Call emergency services without delay: Tell the operator that you suspect a heart attack. They can guide you until help arrives.
Step 2 Sit or lie down in a comfortable position: Do not walk around. Sit on the floor with your back supported, or lie down flat. Minimize physical effort entirely.
Step 3 Loosen tight clothing: Loosen any clothing around the neck, chest, or waist to make breathing easier.
Step 4 Chew aspirin if advised and available: If the person is not allergic to aspirin, is conscious, and emergency services advise it, chewing (not swallowing whole) a standard aspirin tablet can help limit clot formation. Do not do this without guidance.
Step 5 Stay calm and keep the person reassured
Anxiety raises heart rate and worsens strain on the heart. Speak calmly, stay with the person, and wait for emergency services.
Step 6 Be ready to perform CPR
If the person becomes unresponsive and stops breathing normally, begin CPR immediately. Push hard and fast in the centre of the chest — about 100–120 times per minute.
Importance of Quick Medical Response
The medical window for saving heart muscle is remarkably short. Ideally, a blocked coronary artery should be opened within 90 minutes of the first symptoms — this is known as door-to-balloon time in cardiology. Every minute of delay means more heart cells die and cannot be recovered. The long-term difference between a person who reaches the catheterization lab quickly and one who waits hours can be the difference between a full recovery and lasting heart damage.
Do not let embarrassment, uncertainty, or hope that it will “go away on its own” delay emergency care. It is always better to go to the hospital and be reassured it wasn’t a heart attack than to wait at home and miss the critical treatment window.
Risk Factors Linked to Heart Attack Symptoms
Knowing your personal risk factors helps you understand how alert you should be to potential cardiac symptoms. Some risk factors can be changed with lifestyle adjustments; others need ongoing medical management.
Lifestyle-Related Risk Factors
| Risk Factor | Why It Matters | What You Can Do |
| Smoking | Damages artery walls, promotes plaque buildup, increases clot risk | Quit smoking — risk decreases significantly within months |
| Physical inactivity | Leads to weight gain, high blood pressure, poor cholesterol levels | 30 minutes of moderate exercise on most days of the week |
| Poor diet | High saturated fat and processed food intake accelerates plaque formation | Increase vegetables, fruits, whole grains, and healthy fats |
| Excess alcohol | Raises blood pressure and can weaken the heart muscle over time | Limit or avoid alcohol |
| Chronic stress | Persistent stress hormones increase blood pressure and inflammation | Stress management — exercise, sleep, mindfulness, social connection |
| Obesity | Excess weight strains the heart and raises multiple risk factors | Gradual, sustained weight loss through diet and activity |
Medical Conditions That Increase Risk
Certain health conditions significantly raise the likelihood of experiencing cardiac events and make it even more important to learn the symptoms of heart attack early. High blood pressure (hypertension) is one of the most common — it puts constant excessive strain on the artery walls, making them more vulnerable to damage and plaque. High LDL cholesterol encourages plaque buildup inside the coronary arteries over years.
Type 2 diabetes not only raises the risk of heart disease significantly but also blunts the pain signals that would normally warn of cardiac distress. A family history of heart disease — particularly in a parent or sibling who experienced a heart attack before the age of 55 in men or 65 in women — is a strong independent risk factor. Anyone with these conditions should be especially familiar with all the common symptoms of heart attack and should not hesitate to seek help when they arise.
Symptoms Often Mistaken for Heart Attack
Not every chest pain or discomfort signals a heart attack. Several common conditions can produce symptoms that feel alarmingly similar. Understanding these helps you avoid unnecessary panic — but it should never be used as a reason to delay seeking help when you are genuinely unsure.
Acidity or Gas Pain
Gastroesophageal reflux disease (GERD) and trapped gas can cause a burning or pressing sensation in the chest and upper abdomen that mimics cardiac pain. The discomfort from acid reflux often worsens after eating, when lying down, or when bending over. It usually improves with antacids, which is one way to distinguish it from cardiac pain. However, because the two can feel so similar, any chest discomfort that is new, severe, or accompanied by other warning signs should be evaluated medically rather than assumed to be digestive.
Muscle Strain
A pulled or strained muscle in the chest wall (costochondritis) can produce sharp or aching chest pain that gets worse when you press on the chest, move in certain ways, or take a deep breath. Unlike cardiac pain, this discomfort is usually very localized — you can point to exactly where it hurts — and it tends to be worsened by physical pressure or movement. Cardiac chest pain, by contrast, is usually more diffuse and not made worse by pressing on the chest wall.
Panic Attack
A panic attack can produce an alarming set of symptoms: chest tightness, rapid heartbeat, shortness of breath, dizziness, sweating, and a feeling that something is terribly wrong. These closely overlap with the symptoms of heart attack. The key differences are that panic attacks often develop in specific anxiety-provoking contexts, include intense fear or a sense of impending doom, and typically resolve within 20–30 minutes as the attack subsides. Heart attack symptoms tend to be more persistent and often gradually worsen over time. If you are uncertain — and especially if it is your first time experiencing such symptoms — go to the emergency room. A panic attack diagnosis is one of exclusion after cardiac causes have been ruled out.
Conclusion
Your heart works hard for you every single day — the least you can do is listen when it’s trying to tell you something. Understanding the symptoms of heart attack can truly save lives. Whether it’s unusual tiredness, a strange ache in your jaw, or chest discomfort that just won’t quit, never brush off these symptoms of heart attack. Recognizing the early symptoms of heart attack and acting fast can mean the difference between a full recovery and lasting damage. Stay informed, know the symptoms of heart attack, and don’t hesitate to call for help when something doesn’t feel right. Your life — or someone else’s — could depend on it.